Concussions and CTE What You Need to Know 6 Part Series Part 4…Get Part 1 Here
Nutrition is crucial to ensure a safe recovery after a concussion. Since the body goes into an imbalance, it needs some help in putting its processes in balance again. An appropriate amount of energy and nutrition is required to speed up the healing process as well. What you need to eat after a concussion depends on what structural and physiological changes are inflicted by a concussion.
In initial stages, as the previous article explained, the body faces a deficit of proteins, energy and structural constituents like cofactors for various enzymes. To meet this deficit, your diet should be rich in amino acids, proteins, and vitamins. These constituents combine to give your body a strong package of support to come out of the aftermath of a concussion.
“To meet this deficit, your diet should be rich in amino acids, proteins, and vitamins.”
A detailed account of nutritious elements that you need to supplement your diet with is given below:
Antioxidants
One of the initial changes that your body faces after a concussion is an oxidative burden. It is associated with metabolic changes and cellular damage. The free radicals produced as a result of metabolism wreak havoc on normal cells of the body. The brain is particularly vulnerable to the damage of these free radicals. The cellular membranes of neurons need to be protected from these highly reactive species. So, soon after the concussion, the oxidative burden needs to be countered. A diet rich in antioxidants is recommended to ensure the safety of cells and speedy recovery.
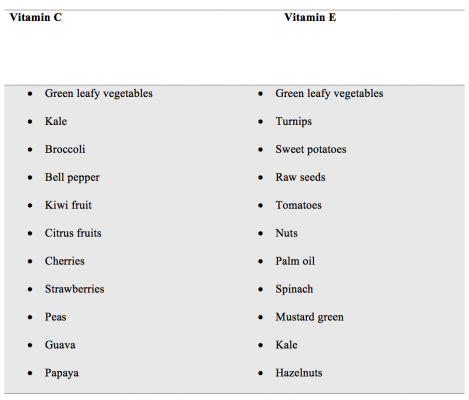
Antioxidants include vitamin E and C. These are naturally present in your body to counter the general harmful impacts inflicted by free radicals. However, research shows that following a brain injury, the levels of these antioxidants, particularly vitamin C, are low in the human body. These levels need to be maintained by supplementing your body with appropriate nutrition. There are many natural fruits and vegetables available that are full of antioxidants. These vitamins enter in your body and directly neutralize the free radicals produced in initial stages of head injury.
“These levels need to be maintained by supplementing your body with appropriate nutrition.”
Food products that contain antioxidants are as follows:
What does the research say?
A controlled clinical trial was done by the American College of Emergency Physicians (ACEP) in 2010 regarding the effects of the antioxidant, vitamin E, which hinted at improvements in TBI patients. High doses of vitamin E were given to the patients who had experienced traumatic brain injuries.
Results displayed a 29% decrease in the mortality rate of the patients as compared to the mortality rates of patients who were put on placebo or high dosages of vitamin C. Although the vitamin C group did not do as well as the vitamin E group… the vitamin C group did show an overall improvement in the healing process and reduction in the size of the injured parts of the brain.
Dr. Ali Razmkon presented this study at the annual meeting of the congress of neurological surgeons. The theory behind his study presented that Vitamin E can reduce the rate of lipid peroxidization and the deficiency of the antioxidant can cause secondary damage in head injuries.
Studies on the effects of antioxidants on brains were done on animals in 2010. Two groups of male rats were fed a regular diet with or without Alpha-tocopherol (vitamin E) for a period of four weeks. This was all given prior to administrating the rodents with a mild fluid percussion injury. The rats were assessed with a Morris water maze.
The group which was given the antioxidant showed a favorable brain status of oxidized proteins and better cognitive function than the group that was left untreated. The protective abilities of Vitamin C were tested once more with guinea pigs as well. The group that was given alpha tocopherol prior to the brain injury showed lower lipid peroxide levels in the traumatized brain tissues.
There has been recent evidence for vitamin C as well that shows effects on the treatment for brain injuries. A treatment was reported in 2005 using a combination of both vitamin C (200mg/day) with an aspirin therapy. The results of the trial showed the group receiving the combination showed significantly lower lipid peroxidization than the control group that was administered with only the aspirin therapy.
Choline
Choline plays a major role in post-concussion brain injury. It has an ability to form components of cellular membranes. So, it repairs them and restores their structural integrity. Choline is also involved in the formation of acetylcholine. Acetylcholine is a neurotransmitter produced in the brain and responsible for coordination. It also helps in the neural development and maintains their functional integrity. These properties of choline make it a healthy option in the outcome of inflammatory, heart and neuronal disorders.
“Choline is also involved in the formation of acetylcholine. Acetylcholine is a neurotransmitter produced in the brain and responsible for coordination.”
Choline is found in eggs and liver. So, a diet rich in these food materials is recommended for patients suffering from a concussion. The scope of choline in healing head injury has been tested by multiple types of research. Studies have shown that choline has special impacts on the human brain. It increases the densities of receptors responsible for binding acetylcholine and dopamine. These chemicals play a major role in memory maintenance. So, choline shows promising results in boosting memory. This makes it a therapeutic option in neurodegenerative diseases like Parkinson’s in which patients have to struggle with severe memory loss. It also ameliorates behavioral and cognitive alterations associated with a head injury.
One major problem in people suffering from head injury is calcium-mediated cell death and apoptosis. These are normal physiological responses initiated in cells after head injury. However, they have collateral damages attached to them because they exacerbate the head injury. Choline helps in putting these responses in control by activating the proteins that stop apoptosis and cell death. It also forms constituents of cell membranes and new brain cells. These productive roles of choline make it a neuroprotective dietary constituent and one of the top recommendations after head injury.
Foods rich in choline include:
- Fish
- Poultry
- Rice
- Spinach
- Nuts
- Pasta
- Mushrooms
- Shellfish
- Liver
- Cauliflower
- Eggs
What does the research say?
Choline Human Trials
The studies carried out to test the effects of Choline on TBI’s, applied the use of phosphatidylcholine, which is also known as CDP-choline. CDP-choline consists of cytidine and choline. The CDP-choline provides the choline needed for the formation of acetylcholine.
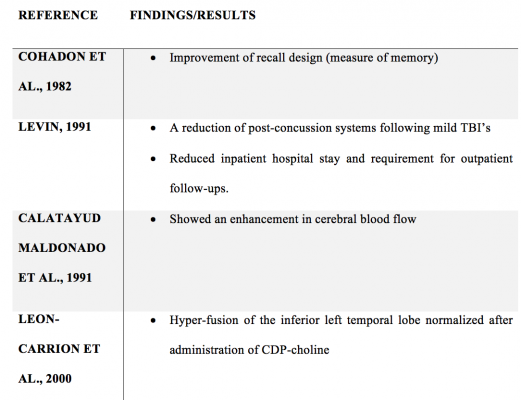
The table below shows early randomized clinical trials of CDP- Choline in TBI patients.
Another randomized trial was done in 2000. The trial subjects were ten patients with severe memory deficits. One group received 1 g/day of CDP-choline, whereas the other was administered with placebo. The CDP-choline group showed improvement in all 5 measures of the neuropsychological treatment that they were being given. Improvements in Verbal fluency and Luria Memory Words were significant.
“The CDP-choline group showed improvement in all 5 measures of the neuropsychological treatment that they were being given.”
One Trial that was done in 1991 showed promising results as well. This trial tested the use of CDP-choline for mild to moderate head injuries. The trial consisted of 14 men divided into two groups. The control group received placebo. The second group was administered 1 g of CDP-choline orally post-injury. Patients that were treated with CDP-choline showed 100% improvement on tests recalling designs than the placebo-treated patients who only showed 29% improvement.
“Patients that were treated with CDP-choline showed 100% improvement on tests recalling designs than the placebo-treated patients who only showed 29% improvement.”
One more 1991 CDP-choline trial that was performed on patients with severe and moderate TBIs, and a GCS (Glasgow Coma Score) between 5 and 1, showed positive findings. The randomized trial was done on 216 patients. One group of the test subjects was given the conventional treatment, whereas the other group was given CDP-choline along with the conventional treatment for their TBI. The patients with CDP-choline had shorter hospital stays than the patients from the control group. There was an overall improvement in all the initial symptoms. The most significant improvement was in character. As well as showing positive results in their initial symptoms they presented better results on their GCS.
“There was an overall improvement in all the initial symptoms.”
A Human trial has been planned since 2009 which deals with the administration of 1000mg of citicoline twice a day for a period of 90 days. The citicoline will be administered either enterally or orally. Based on the previous trials there’s a high chance that the results of this trial will show promising results as well.
Choline Animal Trials
Adult male Sprague-Dawley rats were used in the years 1997, 2000, and 2003 for animal studies regarding the effects of CDP-choline on Traumatic brain injuries. In 1997 the rats were given daily intraperitoneal injections of 100 mg/kg CDP-choline for 18 days, 1 day after the injury was induced. The CDP-choline treated rats had greater latency on their beam balancing test than the saline treated rats. The acetylcholine outflow was significantly increased in the CDP- choline group.
In 2000, post-injury intraperitoneal injections of saline or CDP choline (50, 100, or 400 mg/ kg) were administered 5 minutes and 4-6hours after the injury. The male Sprague- Dawley rats had reduced edema in the cortex with 100 mg/ kg of the CDP-choline. The 400 mg/ kg showed a reduction in both the cortex along with the ipsilateral hippocampus. The CDP-choline treatment proved to be much more effective than the saline treatment given to the control group.
The latest animal study, which was done in 2003, provided promising results as well. The test group of rats was given intraperitoneal injections 100, 200, or 400 mg/ kg of CDP-choline 3 minutes after inducing the injury and 6 hours post-injury. The administration of 400 mg/kg of CDP-choline reduced the neuron loss in the hippocampus. The treatment of the 200 or 400 mg/ kg of CDP — choline reduced the volume of cortical contusion as well. The same rats showed significant recovery in their neurological function by day 7 to 88% of their preinjury levels.
BCAAs
Branched chain amino acids are precursors of excitatory neurotransmitters in the brain like glutamate. They also have an impact on many amino acids that cross the blood brain barrier and form special chemicals in your brain to monitor your brain activity. The amino acids are responsible for cognitive behavior, successful communication between neurons, sleep patterns and many behavioral changes. When a brain injury occurs, the chemical balance of brain disturbs and brain functionality is altered significantly. Many people notice changes in their sleep patterns, moods, and poor general well-being. The excess production of glutamate also plays a harmful role in the aftermath of the injury. Branched chain amino acids are required to set all these things right.
It’s recommended to supplement the diet with branched chain amino acids in the beginning of healing process. Research has shown promising effects of the amino acids on the recovery process in many animals as well as human model studies. They have a special effect on sleep and wakefulness cycles in animals and scientists anticipate that they can help in improving brain function following a concussion. They can improve memory, cognition and overall brain function of patients. These amino acids are also involved in promoting muscle mass and protein synthesis in cells. A boost in protein synthesis ensures the formation of DNA and numerous new cells are formed as a result.
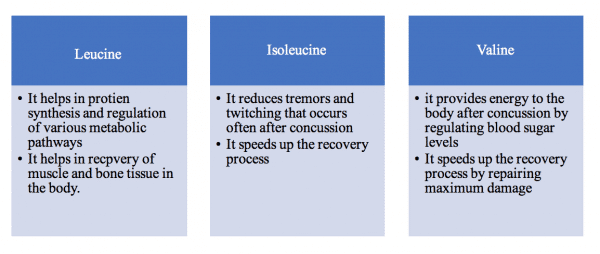
Branched chain amino acids include leucine, isoleucine, and valine. These are found in fruits and vegetables. The individual roles of these amino acids in the body are as follows:
Diet rich in branched chain amino acids include following foods:
- Meat
- Fish
- Lentils
- Nuts
- Egg white
What does the research say?
One prospective randomized clinical study indicates the evidence of the effectiveness of BCAAs for the treatment of TBIs. In 1998, BCAAs were used as an acute treatment for TBIs. Twenty hospitalized brain injured patients were randomized into groups. One group was to be given the standard amino acid formula. The other group was given higher percentages of leucine, isoleucine, and valine (these are branched chain amino acids) included in the standard formula. The patients who were administered the BCAA-enriched formula presented a positive nitrogen balance. The group that had been given the standard formula was in a negative balance.
In 2005, 60 men with severe TBIs were inducted in a randomized placebo-controlled trial. They were administered with BCAA supplements for 15 days intravenously after the injury. After the 15 days of the trial, their Disability Rating Scores (DRS) were tested. Although both the placebo and the treatment groups showed improvement, the group with the treatment of BCAAs showed a more significant improvement.
“Although both the placebo and the treatment groups showed improvement, the group with the treatment of BCAAs showed a more significant improvement.”
Another placebo-controlled study was done in 2008. It consisted of 41 rehabilitation patients with a post-traumatic vegetative or minimally conscious state. The patients were given short-term parental supplementation of BCAAs for 15 days. The DRS (Disability Rating Scale) for the BCAA treated patients showed better improvement, while the score for the placebo-treated patients remained virtually unchanged. Of the BCAA treated patients, 68% achieved DRS scores that allowed them to exit their vegetative or minimally conscious state.
Magnesium
Research has shown an association between low levels of magnesium in the brain and neurodegenerative disease like Parkinson’s. This explains a lot about the concussion patient being vulnerable to the chronic brain problems. Immediately after a brain injury, the magnesium levels drain in your brain and they stay low for at least four days post-concussion. This unavailability of magnesium sets a stage for a reduction in ATP because metabolic pathways that lead to energy production need magnesium as a cofactor. Magnesium also plays important role in activating enzymes required for the recovery process. So, a low level of magnesium needs to be countered after head injury.
Magnesium is involved in initiating membrane potential as well. So, a well-coordinated body becomes impossible in the absence of magnesium. The influx of calcium increases multiple times and calcium-mediated damage happens. The neuronal function also depletes and symptoms of altered behavior surface. To prevent these problems after a head injury, magnesium levels should be raised. The feasible way of doing so is taking a diet rich in magnesium. There is plenty of research ongoing to check the scope of magnesium supplementation in the recovery process and some have shown promising results in humans. One limitation is the crossing of the blood-brain barrier by magnesium. Studies have shown that cerebral flow of magnesium is often halted by the blood brain barrier in humans and that might limit the efficacy of magnesium but other than that, the therapeutic effects are wonderful. Magnesium has also shown promising results in neonates with brain disabilities and this points out its effect as a neuroprotective constituent.
“Magnesium has also shown promising results in neonates with brain disabilities and this points out its effect as a neuroprotective constituent.”
Magnesium supplementation after concussion also limits the damage by maintaining normal body functions. It takes care of energy production and various metabolic pathways. It also reduces inflammation, swelling, and edema in the brain. It ensures maximum coordination and preserves neuronal function. So, what’s stopping you from taking magnesium? Make your diet rich in magnesium and fill your brain with it. Your head trauma will fade away as soon as it ensues.
Foods rich in magnesium include:
- Avocadoes
- Fish
- Nuts
- Green leafy vegetables
- Yogurt
- Dried fruits
- Bananas
- Chocolates
What does the research say?
A test was done to conclude whether treatment with magnesium favorably affected outcomes in head injury patients. A regional trauma center performed a double-blind trial with 499 patients, of ages 14 or older, with severe traumatic brain injuries. The trial took place in August 1998.
The patients were randomly assigned one or two doses of magnesium or placebo within 8 hours of the injury consecutively for 5 days. The outcome of the trial was to be based on a composite of mortality, seizures, functional measures, and neuropsychological tests that were to be assessed up to 6 months post-injury. The group which received a higher dosage of magnesium showed more improvement than those who were being given less magnesium or placebo.
“The group which received a higher dosage of magnesium showed more improvement than those who were being given less magnesium or placebo.”
In another research, Dhandapani et al. 2008 studied the effects of intravenous or intramuscular magnesium sulphate (MgSO4) supplementation in patients with TBI following their head injury.
Following were the results noted:
- At 3 months, the patients treated with MgSO4 had good overall outcomes, like improved recovery, compared to the placebo group. To be precise, 74% of the participants in the MgSO4 group responded well to the treatment compared to only 40% of the placebo group.
- When operated, a significantly higher proportion of the placebo participants showed marked brain swelling (70%) compared to the 30% of the magnesium sulphate group showing brain swelling.
- The overall mortality rate in the placebo group was higher (40%) compared to the MgSO4 group (only 13%).
Delayed Cerebral Ischemia (DCI) is another complication of TBI. DCI is an important risk factor for TBI-related morbidity and mortality. Dorhout et al. 2007 studied the effects of magnesium supplementation on the risk of DCI. Researchers noted that magnesium supplementation lowered the risk of DCI. After 8th day, patients with the lowest serum levels of magnesium were prone to the highest risk of DCI.
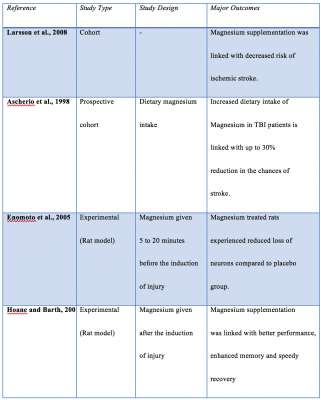
Other research studies are as follows:
Ketogenic Diet
The ketogenic diet is composed of abundant fats but limited carbohydrates. This diet provides an alternative source of energy in the absence of metabolism of glucose. In usual circumstances, glucose is metabolized to form energy. However, in conditions when the body doesn’t have sufficient glucose to convert it into ATP, like in traumatic brain injury, body shifts to oxidation of fats for deriving energy. It happens in body physiologically but you can enforce it artificially too. That’s why a ketogenic diet is recommended after a concussion. Your body faces an energy recession after head injury and an altered energy source is provided by this ketogenic diet.
<<insert graphic19.jpg here>>
Besides being an alternate energy source, ketogenic diet shows efficacy in brain development. Research has shown ketogenic diet is effective in treating epilepsy in children. It has also been used to heal problems like Parkinson’s; hypoxia-induces injury and mechanical trauma in the head. These conditions have similar pathological mechanisms like concussion induced injuries. So, the ketogenic diet is thought to be effective in the healing process of a concussion. It does so by reducing metabolic stress and up-regulating energy levels. The ketogenic diet is also involved in the formation of some inhibitory neurotransmitters like GABA. So, its role in preventing seizures can be anticipated. It also reduces the formation of reactive oxygen species, alleviating the oxidative burden which is supposed to wreak havoc on your body after a concussion.
“…the ketogenic diet is thought to be effective in the healing process of a concussion.”
Ketogenic diet includes:
- Bacon
- Shellfish
- Eggs
- Pork
- Sausage and bacon
- Meat
- Mayonnaise
- Peanut butter
- Avocado
- Macadamia nuts
What does the research say?
Human Trials
There aren’t any human studies on the effects of a ketogenic diet on TBIs. However, we have a lot of well-performed trials that provide proof of positive reinforcement of Ketogenic diet on Childhood epilepsy syndromes.
Studies showed a 50 percent decrease in seizures and an approximate of 15.8% of patients with epilepsy syndromes and partial epilepsy syndromes became free of seizures. Just as well 32% of patients experienced a 90% reduction in the frequency of their seizures. The patients were then given BCAA supplements along with the ketogenic diet which induced an even greater reduction in seizures and three patients experienced a complete cessation of seizures.
Animal Studies
Studies with rat models have been done that have suggested a reduction in the volume of damage and have shown signs of improvement in recovery with the use of the Ketogenic diet on TBIs.
A trial done on Sprague-Dawley rats, ages 17, 35, 45, 65 days showed positive results in 2005. They were administered with a ketogenic diet after a brain-injury was induced. The volume of contusion showed a visible decrease in the rats of the ages 35 and 45 days old.
Two studies were done in 2009 using Feeney’s weight drop model. It was a method used to induce a brain trauma in rats and mice. The trauma from the model uses cortical contusion and damage to the blood brain barrier. In both tests, juvenile male Sprague- Dawley rats were used and divided into groups where one was given a ketogenic diet, and the other was provided with a normal diet. The injury had caused an increased brain edema, but, the intake of the ketogenic diet after the trauma caused a reduction in the brain edema. The ketogenic diet reduced apoptosis in the rats’ brains as well.
“The injury had caused an increased brain edema, but, the intake of the ketogenic diet after the trauma caused a reduction in the brain edema. The ketogenic diet reduced apoptosis in the rats’ brains as well.”
One more study was done in 2009, where Sprague- Dawley rats were induced with controlled cortical impact (CCI). The rats used were either 35 days or 75 days old. Post-injury they were kept on either a ketogenic or standard diet that lasted for 7 days. Their performance on the beam walking test was comparatively different due to the fact that the rats on the standard diet were doing much worse than the rats on the ketogenic diet. The test subjects on the ketogenic diet also presented much fewer foot slips than the rest of the groups.
“The test subjects on the ketogenic diet also presented much fewer foot slips than the rest of the groups.”
Increased oxidative stress following brain injury is another important mechanism that accentuates brain damage and hampers proper healing. One of the main reasons for increased oxidative stress is a decrease in the levels of anti-oxidants, liked glutathione, post-injury.
Jarrett et al. 2008 studied the effects of ketogenic diet on the levels of oxidative stress and anti-oxidants in adolescent male Sprague-Dawley rats. Traumatic brain insult was inflicted and the rats were either given a Ketogenic diet or a control diet for a period of 3 weeks. After 3 weeks, the rat group on Ketogenic diet showed a significant reduction in the levels of oxidative stress and improvement in the brain levels of glutathione.
“After 3 weeks, the rat group on Ketogenic diet showed a significant reduction in the levels of oxidative stress and improvement in the brain levels of glutathione.”
Healing nutrients are so plentiful that we had to break them into two parts. Part 5 of this 6 part series reveals even more of these amazing nutrients.





Reply